Bird allergies in people typically show up as sneezing, a runny or congested nose, itchy and watery eyes, coughing, wheezing, and sometimes skin hives or a rash. These symptoms come from exposure to bird dander, feathers, dried droppings, and the tiny airborne particles all of those shed. Most people notice them within minutes of being around a bird or entering a room where one lives, and they ease up once the exposure stops.
Symptoms of Bird Allergies: What to Do Next

Common bird allergy symptoms in people
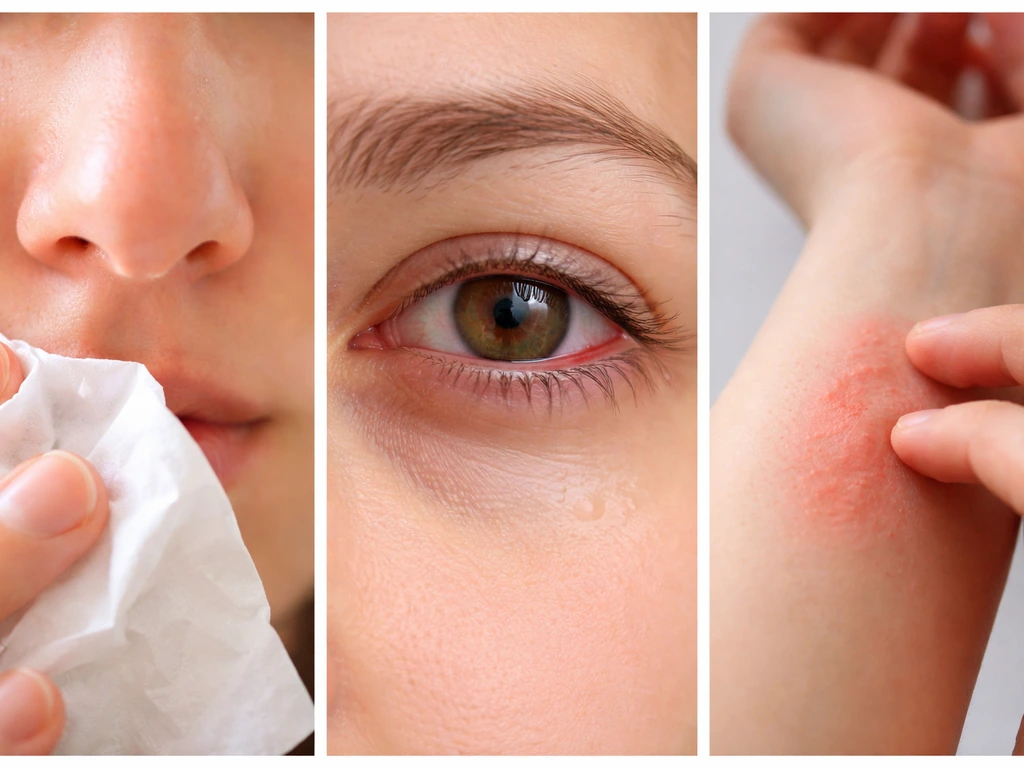
Bird allergy symptoms fall into three main categories: respiratory, eye-related, and skin reactions. They're driven by your immune system overreacting to proteins in bird dander, feather dust, and dried droppings. Here's what each category looks like.
Respiratory symptoms
- Sneezing, often repeatedly and quickly after entering a bird's space
- Runny nose or postnasal drip
- Nasal congestion or stuffiness
- Itching in the nose, roof of the mouth, or throat
- Coughing, chest tightness, or a feeling of not getting enough air
- Wheezing or shortness of breath (especially if you have asthma)
Eye symptoms
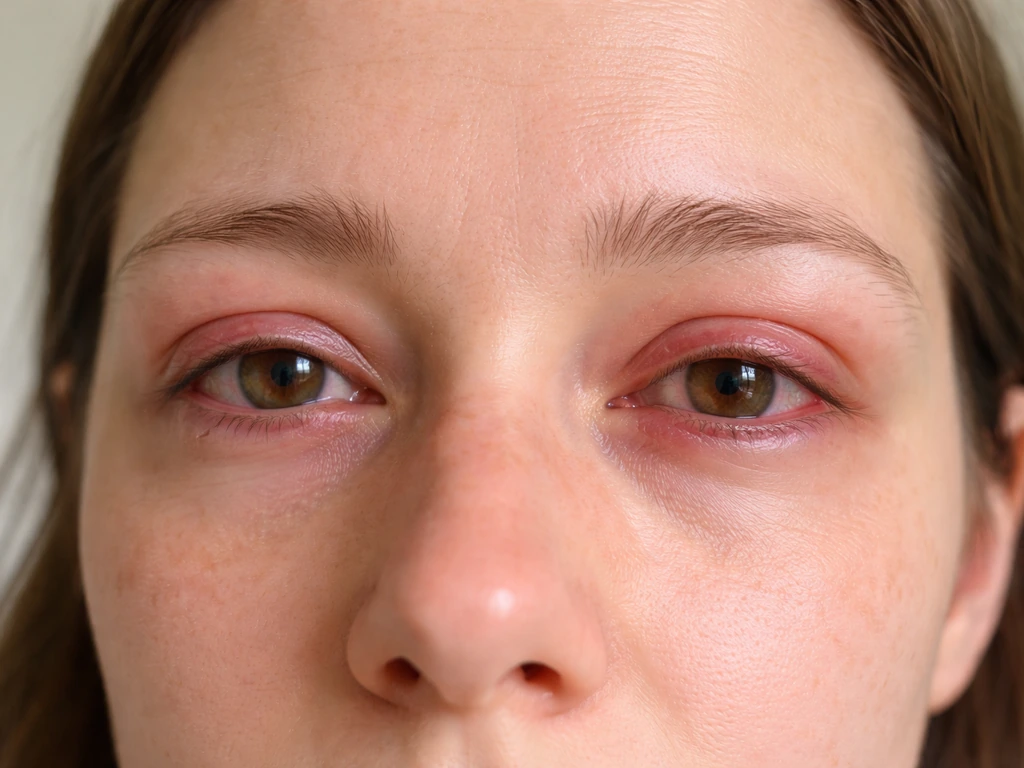
- Itchy, red, or watery eyes
- A burning or gritty feeling in the eyes
- Puffy or swollen eyelids
Skin symptoms
- Hives (raised, discolored, itchy patches) that appear after direct contact or even just proximity to a bird
- A rash or skin irritation from handling a bird directly
- Itching or redness where feathers or dander land on the skin
The nasal and eye symptoms tend to look a lot like hay fever, which makes sense because the underlying mechanism is the same. Your body releases histamine and other chemical mediators in response to the allergen, and those chemicals cause the swelling, itching, and fluid production you feel.
When symptoms show up and what triggers them
The timing and pattern of your symptoms can tell you a lot about what's going on. Classic IgE-mediated bird allergies (the standard immune-response type) tend to start fast, usually within minutes of exposure. You walk into a room with a parrot, a cockatiel, or even a cage that hasn't been cleaned recently, and your eyes start itching or your nose starts running almost immediately.
Pet birds vs. wild bird exposure

Pet birds, especially parrots and cockatiels, are heavy producers of fine feather dust and dander. You get continuous, close-range exposure at home, which is why symptoms often feel constant or get worse over time. Wild bird exposure tends to be more intermittent, like cleaning out a bird nest in your gutters or spending time in an aviary, but those short, concentrated exposures can hit just as hard. If you suspect a bird nest allergy, knowing these bird nest allergy symptoms can help you spot them early and decide what to do next. Bird dust allergy symptoms and bird dander allergy symptoms both follow this same fast-onset pattern when the trigger is a typical IgE allergic response.
The main triggers
- Bird dander (tiny skin flakes shed continuously)
- Feather dust and down, especially from powder-down birds like cockatoos and African greys
- Dried droppings, which release particles into the air when disturbed
- Airborne proteins from feathers or droppings that settle on surfaces and get stirred up during cleaning
Worth knowing: there's a separate, more serious condition called hypersensitivity pneumonitis (sometimes called bird fancier's lung) that's triggered by the same sources but follows a delayed timeline. Acute symptoms typically develop 4 to 8 hours after exposure, often after you've already left the area. That means you might feel fine around the birds, then develop fever, chills, muscle aches, cough, and shortness of breath hours later at home. That's a different immune reaction than a standard bird dander allergy, and it deserves its own evaluation.
Is it a bird allergy or something your bird is dealing with?
This is a genuinely important question if you're a bird owner. Respiratory symptoms around a bird don't automatically mean you're allergic. There are a couple of bird-related illnesses that can cause respiratory symptoms in the people around them, and you need to be able to tell them apart. Bird bite infection symptoms can include increasing redness, warmth, swelling, and pain around the bite, sometimes with fever or pus. If your bird seems uncomfortable, look out for bird ear infection symptoms such as head shaking and discharge.
Allergy vs. infection: the key differences
| Feature | Bird Allergy (in you) | Psittacosis / Infectious illness (in you) | Hypersensitivity Pneumonitis (in you) |
|---|---|---|---|
| Onset after exposure | Minutes | Days after exposure to infected bird | 4 to 8 hours after leaving area |
| Fever and chills | No | Yes, often prominent | Yes, in acute attacks |
| Nasal/eye itching | Very common | Uncommon | Uncommon |
| Sneezing and runny nose | Common | Less typical | Less typical |
| Muscle aches/headache | No | Common | Can occur |
| Cough and shortness of breath | Possible, especially with asthma | Yes | Yes, prominent |
| Improves away from birds | Yes, quickly | Requires antibiotic treatment | Improves but may take days |
Psittacosis, sometimes called parrot disease, is a bacterial infection people can get from breathing in dust from dried bird droppings or respiratory secretions from an infected bird. It's not an allergy, and it doesn't respond to antihistamines. If someone in your household develops flu-like symptoms including fever, headache, and dry cough after handling a sick bird or cleaning a cage, that's a reason to see a doctor and mention the bird exposure clearly. The same goes for bird infection symptoms you might notice in the bird itself, like labored breathing, discharge, or lethargy, which should prompt a vet visit.
The quick rule of thumb: if your symptoms are mostly itching, sneezing, and runny eyes that clear up when you leave the bird's space, that points toward allergy. If you're running a fever, feeling like you have the flu, or symptoms are getting worse over days despite being away from the birds, something else is going on and you should see a doctor.
How bird allergies are diagnosed
There's no single definitive bird allergy test, but clinicians piece together the picture from a few different sources.
Exposure and symptom history
The most important starting point is your history. A clinician will want to know when symptoms started, whether they correlate with being around birds, whether they improve when you leave the environment, and whether they've gotten worse over time. Keep a mental note (or a written one) of which situations trigger symptoms, how fast they start, and how long they last. That pattern is often enough to point strongly toward a bird allergy diagnosis.
Allergy testing
When the history isn't clear or if treatment isn't working, a clinician may order allergy testing. Two main options exist: skin prick testing and blood tests that measure allergen-specific IgE antibodies. Both look for evidence that your immune system has been sensitized to specific proteins, such as those from feathers or bird dander. Testing helps confirm the specific trigger, which is especially useful if you're around multiple animals or if you want to consider allergen immunotherapy (allergy shots) down the road.
For suspected hypersensitivity pneumonitis, the workup looks different and typically involves lung function testing, imaging, and detailed exposure history rather than standard IgE allergy panels. If your symptoms include the delayed fever-and-cough pattern described earlier, mention that to your doctor specifically.
When symptoms become an emergency
Most bird allergy symptoms are uncomfortable but not dangerous. However, there are situations where you need to act fast.
Severe asthma flare
If you have asthma and bird exposure triggers a flare, it can escalate quickly. Wheezing that doesn't improve with your rescue inhaler, increasing chest tightness, or significant difficulty breathing are signs to seek urgent care or call emergency services rather than waiting it out.
Anaphylaxis
Anaphylaxis from bird exposure is rare but possible. It's a sudden, severe allergic reaction that involves multiple body systems at once. If you or someone else develops any combination of the following after bird exposure, call emergency services (911) immediately:
- Hives or widespread itching combined with trouble breathing
- Swelling of the lips, mouth, tongue, or throat
- Chest tightness plus dizziness, lightheadedness, or a racing heart
- A sudden drop in blood pressure or feeling of impending collapse
- Vomiting or diarrhea alongside breathing difficulty
If epinephrine (an EpiPen) is available and anaphylaxis is suspected, use it and still call 911. Don't assume the injection alone is sufficient to handle the reaction.
Hypersensitivity pneumonitis warning signs
If you're repeatedly exposed to bird allergens and your symptoms are getting progressively worse over weeks or months (shortness of breath, persistent cough, fatigue, weight loss), that's a sign that the lung condition may be progressing from acute to chronic. Severe cases can require hospitalization. Don't ignore a cough and breathlessness that just keeps building up even after you reduce exposure.
What you can do today for relief and prevention
Avoidance is the single most effective strategy, but it's also the one people are least willing to follow, especially when a bird is a beloved pet. If rehoming the bird isn't something you're considering, these practical steps can meaningfully reduce your exposure and symptoms.
Reduce exposure at the source
- Keep the bird in one room and restrict it from bedrooms and main living areas where you spend the most time
- Have someone without bird allergies handle cage cleaning whenever possible
- When you do clean the cage, wet down droppings and feathers before wiping rather than dry-sweeping or shoveling, which sends particles airborne
- Wash your hands and change your clothes after handling the bird or cleaning its space
- Bathe the bird regularly if it tolerates it, since bathing reduces the dander load it sheds
Improve the air quality in your home
- Use a HEPA air purifier in the room where the bird lives and in your bedroom
- Replace standard HVAC filters with high-efficiency filters and change them more frequently
- Keep windows open when weather allows to improve ventilation, especially during and after cage cleaning
- Vacuum regularly with a HEPA-filter vacuum to capture settled dander and feather particles from floors and furniture
Medications to discuss with a clinician
Several medication options can help manage ongoing symptoms. These are worth talking through with a doctor or allergist rather than just grabbing whatever is on the pharmacy shelf, because the right choice depends on your specific symptom pattern.
- Antihistamines: oral antihistamines help with itching, sneezing, runny nose, and hives. Non-drowsy options are available over the counter.
- Intranasal corticosteroid sprays: for moderate to severe nasal symptoms, steroid nasal sprays are often the most effective first-line treatment according to clinical guidelines.
- Combination nasal sprays: products combining an antihistamine and a steroid are available for people who need better control than a single agent provides.
- Eye drops: antihistamine eye drops can relieve itchy, watery eyes directly.
- Prescription options: if over-the-counter approaches aren't enough, a clinician may discuss prescription-strength medications or referral to an allergist for possible immunotherapy.
For hypersensitivity pneumonitis specifically, eliminating or drastically reducing exposure to the triggering particles is the primary treatment. Medications may be used when symptoms don't resolve after reducing exposure, but that's a conversation for a doctor who can assess your lungs properly.
If you're a bird owner trying to manage ongoing bird allergy symptoms in yourself or someone in your household, the combination of source control, air filtration, and appropriate medication will get you the furthest. Start with the cleaning and air quality changes today while you arrange a medical appointment to confirm the diagnosis and get a proper treatment plan in place.
FAQ
Can symptoms of bird allergies happen without sneezing or itchy eyes?
Yes. If you have asthma, bird exposure can trigger bronchospasm even if you do not get typical itchiness or watery eyes. Pay close attention to symptoms like chest tightness, wheezing, reduced exercise tolerance, and rescue inhaler use increasing after bird contact.
If I take allergy medicine, how do I know whether it is truly a bird allergy?
Antihistamines may help itching, sneezing, and runny nose, but they do not treat hypersensitivity pneumonitis or psittacosis. If you develop delayed fever, chills, muscle aches, or worsening shortness of breath hours after exposure, focus on getting medical evaluation rather than relying on allergy meds.
What timing pattern most strongly suggests classic bird allergies versus bird fancier’s lung?
Watch for the timeline. IgE-mediated allergy symptoms usually start within minutes and improve after leaving the room, while hypersensitivity pneumonitis often begins 4 to 8 hours later and can worsen after you are already home.
Why do my symptoms sometimes continue even after I leave the house with a bird?
Airborne triggers can linger, especially in bedding, carpets, and HVAC returns, so “leaving the room” may not bring instant relief. Consider whether symptoms persist longer than expected (for example, more than a few hours) and whether there are dust sources like unsealed bird cages, feather storage, or dirty filters.
Are the triggers different if symptoms happen mainly during cage cleaning?
If the onset is after you clean cages, handle droppings, or disturb nests, you may react to dried droppings or feather dust rather than feathers alone. A useful detail to share with your clinician is whether symptoms happen during cleaning, including how fast they begin once you start.
How can I tell bird allergy symptoms from a contagious illness?
It can be confusing. Repeated bird exposure can cause both allergy symptoms and infections in the household, for example if someone is sick or the bird is ill. If symptoms are accompanied by fever, pus-like eye drainage, or rapidly spreading skin redness, treat it as more than “just allergies” and get checked.
Can bird allergies cause delayed breathing symptoms that start hours later?
Yes. Consideration for a delayed lung reaction is important if you experience fever or shortness of breath later in the day after bird exposure, even if you otherwise feel fine initially. Mention the delayed pattern explicitly, since standard allergy panels do not diagnose hypersensitivity pneumonitis.
If I’m allergic to one bird, will I likely react to other birds or unrelated allergens?
Cross-reactivity is possible, meaning you could be sensitive to proteins from other birds or related allergens, and you might also have typical environmental allergies like seasonal pollen. If you have symptoms around multiple animals, ask your clinician whether testing should include a broader allergy panel based on your history.
If an EpiPen is available, do I still need emergency care for anaphylaxis from bird exposure?
Epinephrine is the right choice for suspected anaphylaxis, but you still need emergency care. Use the device immediately if symptoms involve multiple body systems, then call emergency services, even if symptoms improve.
When should I worry that my bird-related symptoms are getting chronic?
Some people confuse “allergy” with “bird ownership.” If symptoms are progressive despite reducing exposure, or you have persistent cough, ongoing breathlessness, or unexplained fatigue or weight loss, do not assume it is simple rhinitis. Those signs warrant prompt medical evaluation for lung involvement and other conditions.
What are common mistakes that make bird allergy symptoms harder to control at home?
Common setup mistakes include cleaning without protection, using feather or nest materials that increase dust, and skipping HEPA filtration or not changing HVAC filters. For self-management, ask your clinician or allergist which combination of source control steps (mask use during cleaning, HEPA placement, filter upgrades) best matches your symptom pattern.
Bird Allergy Symptoms Signs: What to Look For and Next Steps
Spot bird allergy symptoms signs like sneezing, wheeze, itchy eyes and hives, plus next steps and when to get help.


