If a bird has bitten you and the wound is becoming more red, warm, swollen, or painful in the hours after, that's the earliest sign of infection. Redness that spreads beyond the original bite, pus or cloudy drainage, red streaking moving away from the wound, or the appearance of fever and chills means the infection is progressing and you need medical care soon. Most infected bird bites show clear signs within 24 to 48 hours, so that's the window to watch closely.
Bird Bite Infection Symptoms: What to Watch and Do
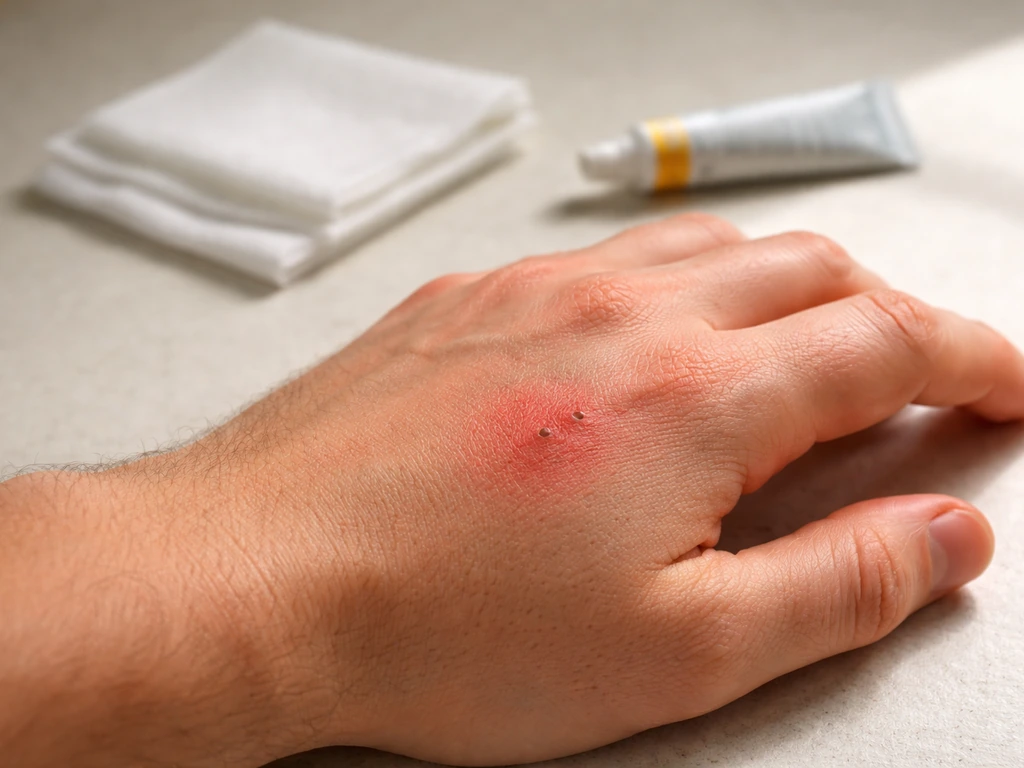
What an infected bird bite looks like: symptom checklist
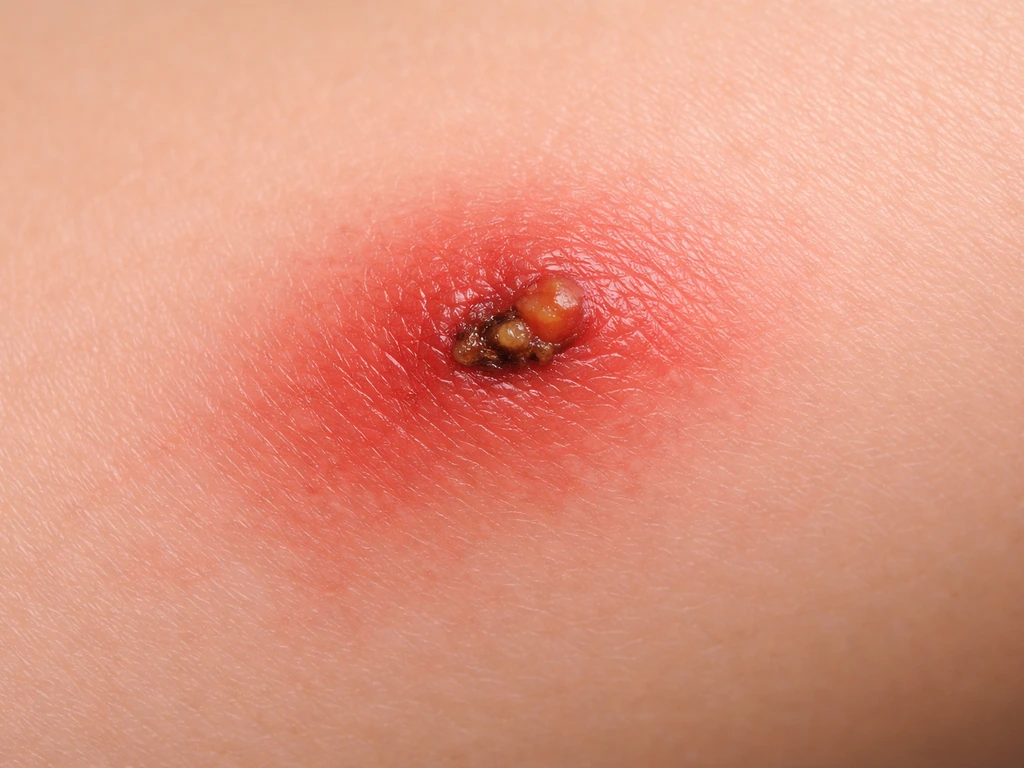
Infection signs fall into two categories: what you see and feel at the wound itself, and how your whole body starts to respond. Here's what to look for.
Local wound signs (at the bite site)
- Redness that is spreading or growing larger over time
- Warmth around or beyond the wound edges
- Increasing swelling and puffiness (not just the initial reaction)
- Pain that is getting worse rather than improving
- Pus, cloudy fluid, or yellow/green drainage from the wound
- An open sore that is not closing or healing
- Red streaks extending outward from the bite (a sign of lymphangitis)
- Blistering, or skin that looks dark, purple, or black (a more serious tissue sign)
Whole-body (systemic) signs

- Fever (100.4°F / 38°C or higher)
- Chills or shaking
- Fatigue or feeling generally unwell
- Swollen, tender lymph nodes near the bite (under the arm for a hand bite, in the groin for a leg bite)
- Rapid heart rate or confusion (these are more serious signs)
One important thing to know: systemic signs like fever and rapid heart rate can appear before the skin around the wound even looks that bad. The IDSA has noted that these whole-body symptoms can sometimes precede visible skin changes. So don't wait for the wound to look alarming before taking fever or chills seriously.
Immediate first aid: what to do right now
The single most important thing you can do immediately after a bird bite is wash the wound thoroughly. Run the bite under clean, running water with mild soap for at least 3 to 5 minutes. Some guidance from the WHO and LA County health departments recommends up to 15 minutes of washing, especially if you are concerned about what the bird may have been exposed to. This step genuinely reduces the bacterial load in the wound and lowers your infection risk.
After washing, apply a thin layer of over-the-counter antibiotic ointment (like bacitracin or Neosporin, unless you have a sensitivity to these), then cover the wound with a clean bandage or dressing. Change the dressing daily and whenever it gets wet or dirty.
If the wound is bleeding significantly, apply gentle pressure with a clean cloth first until the bleeding slows, then move on to washing. Do not skip the washing step even if the bite looks minor. The CDC specifically notes that germs from bird bites and scratches can spread even when the wound does not appear deep or serious.
What not to do
- Do not skip washing because the wound looks small or shallow
- Do not squeeze or press on the wound to force out fluid, which can push bacteria deeper
- Do not apply alcohol or hydrogen peroxide directly inside the wound as a primary cleaner — these can damage tissue
- Do not ignore the wound and assume it will resolve on its own without any monitoring
Red flags and timelines: infected vs. not infected
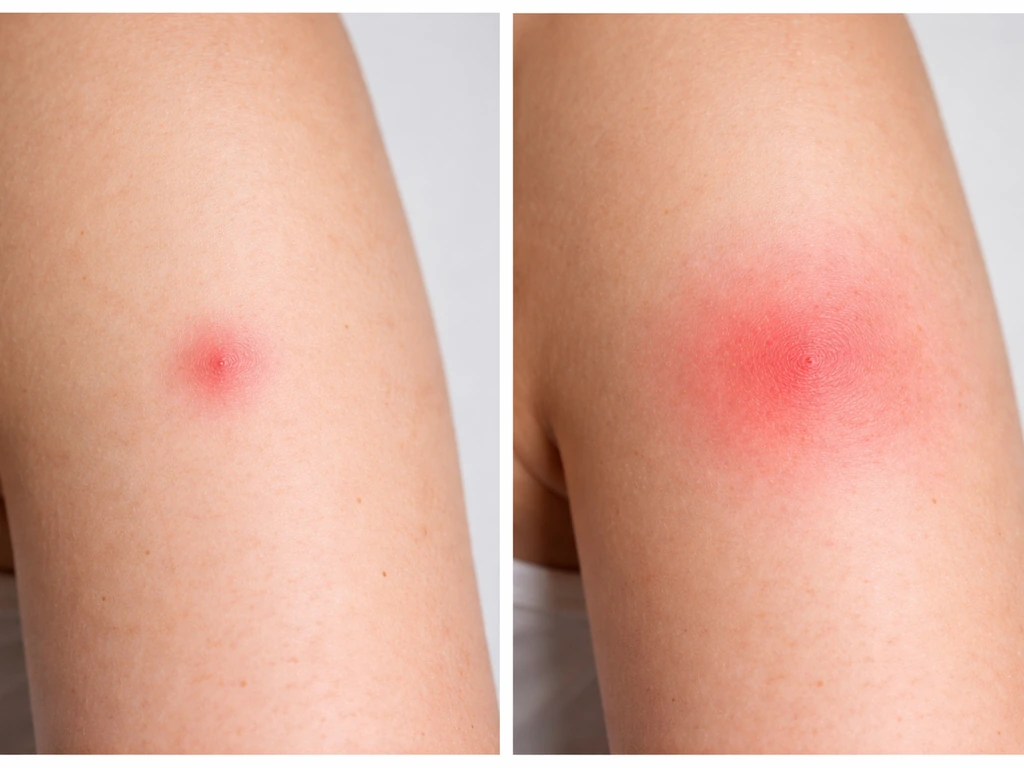
Some redness and mild soreness right after a bite is completely normal. That is your body's inflammatory response, not infection. The difference is the trajectory: normal irritation levels off and starts to improve within a day or so, while infection gets progressively worse.
Infections typically become apparent within 24 to 48 hours of the bite. If you are past that window and the wound looks calm, is not spreading, and you have no fever, that is a reassuring sign. If things are still getting worse at 24 hours, treat it as infection until proven otherwise.
| Sign | Likely Normal Reaction | Likely Infection |
|---|---|---|
| Redness | Limited to immediate bite area, fading within 24 hours | Spreading beyond wound edges, worsening over time |
| Swelling | Mild puffiness at bite site, improving | Increasing or spreading swelling |
| Pain | Sore right after the bite, easing off | Pain intensifying hours or days later |
| Warmth | Slight warmth at site initially | Noticeable, spreading warmth |
| Drainage | Clear fluid or minor bleeding initially | Pus, cloudy, or colored discharge |
| Fever | None | 100.4°F (38°C) or above |
| Red streaking | None | Lines radiating from wound toward the body |
Red streaking extending from the bite is one of the more urgent signs. It indicates the infection may be moving through your lymphatic system, which is a reason to seek care the same day rather than wait.
Local wound signs vs. whole-body infection signs
A localized infection stays at the wound site: redness, warmth, swelling, pain, and possible pus. This is still a problem that needs treatment, but it is contained. A systemic infection means bacteria have moved beyond the wound and into your lymph nodes, bloodstream, or body broadly. That is a more serious situation.
The jump from local to systemic can happen faster than people expect. Cellulitis (a spreading bacterial skin infection) that involves two or more signs of a systemic inflammatory response can meet the criteria for sepsis. That is an emergency. If someone bitten by a bird develops fever plus rapid heart rate, confusion, or unusually low blood pressure alongside wound signs, that combination warrants emergency care immediately, not a wait-and-see approach.
It is also worth knowing that what feels like an infection can sometimes be something else. An <a data-article-id="CBF99CF5-0BEB-49C2-801E-FF92B03892D2"><a data-article-id="C7EE7489-4072-40D7-87C6-3754331B79F1">allergic reaction to bird saliva or proteins in the wound</a></a> can cause localized swelling and itching that mimics early infection. Similarly, if you have bird allergy sensitivities, skin irritation near a scratch or bite can look inflammatory without being infected. The key distinguishing factors are fever, progressive spreading of redness, and pus: those point clearly toward infection rather than allergy or irritation. If you suspect the reaction is not infection but instead matches bird nest allergy symptoms, focus on allergy-type signs like itching and swelling rather than pus or spreading redness. If you are dealing with allergy concerns, compare these wound changes with bird allergy symptoms signs, since allergic reactions can mimic early infection.
Pet bird vs. wild bird bites: does it change the risk?
Yes, the source of the bite matters for how you think about risk, though the first aid steps are the same regardless.
Pet bird bites

A bite from your own indoor pet bird (a parrot, cockatiel, or similar) generally carries lower infection risk than a wild bird bite. The bird's known health status, diet, and environment reduce some variables. That said, bird beaks and mouths do carry bacteria, and even a pet bird bite that breaks the skin needs to be washed promptly and monitored. Do not assume a small bite from a tame bird is automatically harmless.
Wild bird bites
A bite from a wild bird (a pigeon, crow, raptor, or any bird you caught or handled outdoors) raises the infection stakes. Wild birds carry a broader range of environmental bacteria and pathogens. Their beaks and claws may have been in contact with soil, feces, carrion, or other animals. Wash thoroughly and seek medical evaluation sooner rather than later, especially if the bite is deep or the wound looks even slightly concerning.
One important note for those who worry about rabies: according to DC Health and public health authorities, birds do not get rabies. You do not need to pursue rabies post-exposure prophylaxis after a bird bite. This is different from bats, raccoons, or other mammals. That said, other pathogens transmitted via bird bites and scratches are still a real concern, so prompt wound care and monitoring remain important.
Tetanus is worth considering for any bite from an animal. Bird bites involving saliva, soil, or feces are considered higher-risk wound types. If your tetanus vaccination is not current (generally a booster every 10 years, or 5 years for dirty wounds), mention this when you seek medical care. Providers will assess your vaccination history as part of evaluating the bite.
When to get urgent care and what to expect
MedlinePlus recommends seeking medical attention within 24 hours for any bite that breaks the skin. That is a reasonable baseline. But there are situations where you should go sooner or immediately.
Go to urgent care or your doctor within 24 hours if:
- The bite broke the skin and you have not had a tetanus shot in the past 5 to 10 years
- Redness, warmth, or swelling is visible and increasing
- The bite is on your face, hand, or over a joint (these areas carry higher complication risk)
- The bite is from a wild bird or a bird of unknown health status
- You are immunocompromised, diabetic, or have a condition that affects wound healing
Go to an emergency room right away if:
- Bleeding is not controlled after 10 minutes of pressure
- You can see muscle, tendon, or bone in the wound
- Red streaking is extending from the wound
- You have fever plus rapid heart rate, confusion, or difficulty breathing
- The wound is extremely painful out of proportion to its appearance
- You feel suddenly much worse in the hours after the bite
What happens at the appointment
The provider will examine the wound, check the extent of redness and swelling, assess whether there is pus or drainage, and ask about your tetanus vaccination history. For a straightforward localized infection, they may prescribe oral antibiotics and tell you to return or seek emergency care if symptoms worsen. Routine wound cultures are generally not done for typical uncomplicated cellulitis, but if there is an abscess, unusual presentation, or the infection is not responding to treatment, a wound culture may be taken before starting or switching antibiotics to identify the specific bacteria involved. More serious presentations, including any systemic signs, may require intravenous antibiotics or hospital admission.
How to prevent future bites and lower infection risk
Most pet bird bites happen during handling, especially when a bird is stressed, threatened, or overstimulated. Learning to read your bird's body language (feathers fluffed, eyes pinning, posture stiffening) gives you a few seconds of warning before a bite. Approach from the side rather than directly toward the head, and avoid reaching into a cage when a bird is clearly agitated.
For wild bird handling (in rescue or wildlife contexts), thick gloves rated for bird handling reduce both bite force and scratch depth. Even with gloves, wash your hands thoroughly after any handling session.
Keep a small first aid kit accessible in your bird room or wherever you handle birds regularly. Having soap, antibiotic ointment, bandages, and clean gauze immediately at hand means you can treat a bite within seconds instead of searching for supplies. That immediate washing is genuinely protective.
Keeping your tetanus vaccination current is a simple background protection for anyone who regularly handles birds, whether pet or wild. It takes one appointment and removes a variable from the risk equation entirely.
If you are a regular bird owner or caretaker who also deals with respiratory symptoms around birds, it is worth knowing that inhaled bird particles (dander, dust, droppings) can cause entirely separate health concerns that look different from a wound infection. If you are also looking for bird aspiration symptoms, watch for breathing problems that can suggest inhaled material getting into the airway respiratory symptoms around birds. If you are noticing ear discomfort or swelling after being around birds, the bird ear infection symptoms to watch for are similar to other local wound infection signs. Bird dust allergy symptoms often include sneezing, a runny or stuffy nose, itchy or watery eyes, coughing, and wheezing. Those are distinct issues from bite-related infection, but they are worth understanding alongside bite safety as part of overall avian health awareness.
FAQ
How can I tell if bird bite infection symptoms are actually normal irritation?
Not necessarily. If the redness is staying small, not spreading, and you do not develop pus, worsening warmth, or fever, it can be normal irritation from the bite and first aid. As a practical rule, mark the edge of the redness with a pen and recheck in 2 to 4 hours, spreading beyond that border suggests infection rather than simple inflammation.
What if my bird bite seemed better at first, then got worse again?
Yes, worsening can occur even if you start improving. Rewash the wound if you notice new drainage or increasing tenderness, then contact a clinician if redness continues to spread after 24 hours or if you develop fever, chills, or red streaking. This “second wave” often means bacteria were not fully cleared initially or the wound was repeatedly contaminated.
Can a small-looking bird bite still cause a serious infection?
A bite with a puncture may look minor but still become infected. Deeper bites, especially those that break the skin and create a tight scab or trapped wound pocket, can develop cellulitis or abscess even when surface swelling is limited. If pain is increasing or you see any drainage or lymph red streaks, get evaluated sooner.
Does pus or drainage mean I definitely need antibiotics or drainage?
If you are seeing pus, cloudy drainage, or a new lump that is increasingly painful, that suggests possible abscess formation. Abscesses often need drainage and may require a different treatment plan than straightforward cellulitis. Avoid squeezing the area, and arrange prompt medical assessment if these signs appear.
When should I stop monitoring and get same-day medical care?
After proper washing and covering, you can usually monitor at home if symptoms are mild and not progressing. Seek same-day care if you have red streaking, rapidly expanding redness, fever or chills, numbness or severe pain out of proportion to the bite, or if the bite is on the hand, face, genitals, or near a joint. Those locations and symptom patterns tend to worsen faster.
Can bird bite infection symptoms show up in my body before the skin looks infected?
It can. Localized redness and warmth can be subtle early, while systemic signs like fever, chills, and rapid heart rate can show up before obvious skin changes. If you develop any whole-body symptoms, treat it as possible infection and get evaluated even if the wound looks only mildly irritated.
Why are red streaks from a bird bite considered urgent?
Red streaking is a strong reason to be seen urgently because it suggests spread through lymphatic channels. If streaks are present, do not wait for it to “settle,” because that increases the chance you will need prescription treatment promptly.
How do I distinguish an allergic reaction from bird bite infection symptoms?
Not all reactions are infections, allergic or irritant reactions can cause itching, localized swelling, and redness soon after the bite, and they may improve with time rather than progressively expand. Allergy-type presentations usually feature significant itching and may lack fever, pus, and spreading redness over hours. If you are unsure, especially with fever or progressive spreading, choose medical evaluation.
What symptoms mean my bird bite could be sepsis?
Seek emergency care immediately if you have confusion, fainting, unusually low blood pressure, severe weakness, or a combination of fever with rapid heart rate, particularly alongside worsening wound redness or red streaking. These patterns can meet criteria for sepsis and need urgent treatment, even if the wound itself seems only moderately inflamed.
Are there common home mistakes that make bird bite infections more likely?
Don’t rely on home remedies like soaking, hydrogen peroxide, or tight bandaging as a substitute for wound cleaning and monitoring. Hydrogen peroxide and harsh antiseptics can irritate tissue and delay healing, and soaking can keep the wound wet and contaminated. Stick to thorough running-water washing, then a clean, dry dressing.
Is it always necessary to see a clinician within 24 hours after a bird bite?
You should have medical evaluation within 24 hours if the bite breaks the skin, especially for puncture wounds, bites to higher-risk areas (hand, face, genitals), immunocompromised people, or if your tetanus shot is not up to date. Even if you can’t see infection yet, a clinician can assess depth, bleeding risk, and vaccination needs.
What should I tell the clinician about tetanus, and why does it matter?
If you are due for a tetanus booster, mention the injury type and your last vaccination date. For people with unknown or incomplete vaccination history, clinicians may recommend tetanus immune globulin in addition to a vaccine. Bring this detail up early rather than waiting for symptoms.
Do I need to be more urgent if I have diabetes or a weakened immune system?
Seek care sooner if you have diabetes, chronic kidney disease, poor circulation, immune suppression, or you are on medications that weaken the immune system. In these situations, typical wound redness can progress faster, and clinicians may choose earlier antibiotics and closer follow-up.
Can bird-related respiratory symptoms be confused with an infection from a bite?
Yes. If you recently handled birds and also have breathing problems, those may be separate from wound infection. If you have wheezing, shortness of breath, or worsening cough, treat it as an urgent respiratory issue and seek medical care, while still monitoring the wound for red streaking, pus, fever, or spreading redness.
Symptoms of Bird Allergies: What to Do Next
Spot bird allergy symptoms like sneezing, wheeze, itchy eyes, rashes and know next steps, triggers, and when to get help


