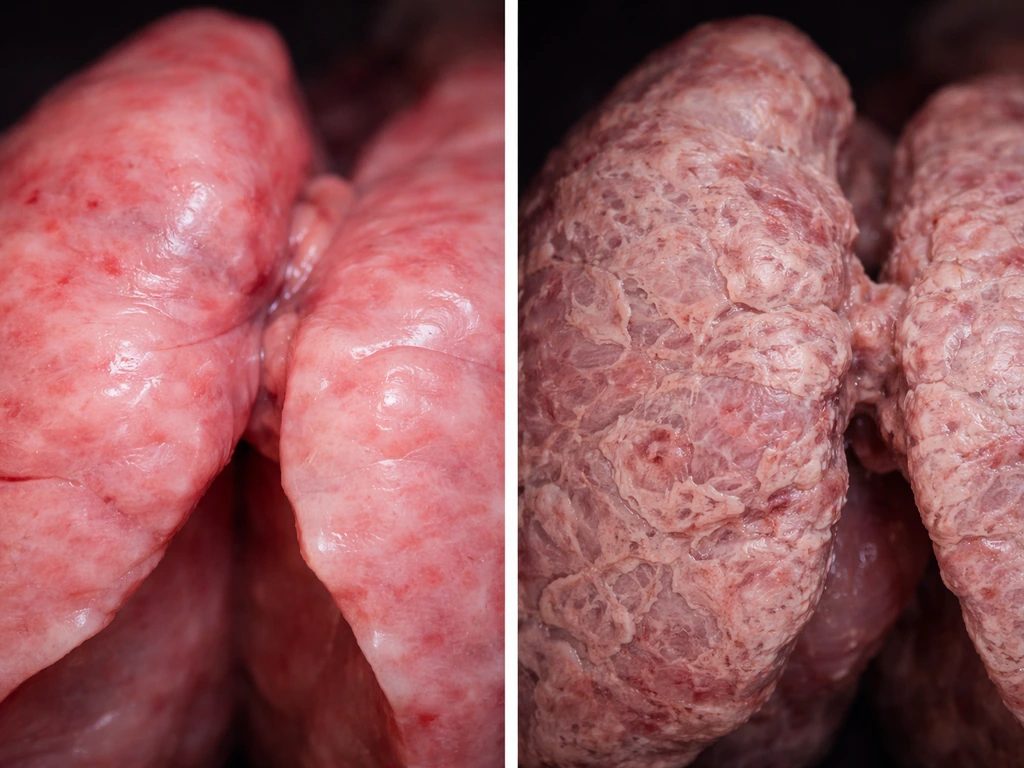
The single most important thing you can do right now, before anything else, is stop or dramatically reduce your exposure to birds, bird droppings, feathers, and any feather-containing items in your home. That action drives almost everything else in terms of recovery.
What bird fancier's lung actually is
Bird fancier's lung is a form of hypersensitivity pneumonitis (HP), which is an immune-mediated reaction where your lungs overreact to an inhaled antigen. It is not an infection and it is not a simple allergy like hay fever. Your immune system mistakes proteins from birds as a serious threat and mounts an inflammatory response inside your lung tissue every time you breathe those particles in.
The specific triggers tied to bird exposure include avian droppings, bird serum proteins, feathers, dust from pet birds, and feather-containing household items like pillows, duvets, and down-filled bedding. You do not have to own a bird to develop it. Living with feather bedding or spending time around pigeons, parrots, cockatiels, or other birds is enough repeated exposure for susceptible people.
Doctors now classify HP into two main types: nonfibrotic and fibrotic. This distinction matters more than whether symptoms appeared suddenly or gradually, because the presence or absence of fibrosis is what predicts how well someone will recover. Nonfibrotic HP has the best chance of full recovery after exposure stops. Fibrotic HP, where scar tissue has built up in the lungs, is progressive and irreversible.

Acute attacks typically develop 4 to 8 hours after a period of heavy exposure. The symptoms feel a lot like a flu hit you out of nowhere: fever, chills, muscle aches, cough, chest tightness, and shortness of breath. They can clear up within 12 hours to a few days if you get away from the source, which is part of why this condition gets missed. People feel better and assume it was a passing illness.
In subacute and chronic forms, symptoms develop more gradually over days to weeks and tend to be more persistent. You might notice a dry cough that won't go away, progressive breathlessness during exercise, fatigue, and unintentional weight loss. Chronic disease can become severe enough to require hospitalization. A key pattern worth noting: if your symptoms improve when you leave home or avoid your birds for a few days and then return when you come back, that cycle is a significant clue.
The timing and exposure pattern are important details to track before you see a doctor. Note when symptoms start, how long they last, and whether they correlate with time spent near birds or bird-related items. That history becomes central to diagnosis.
How doctors confirm it and rule out other conditions
There is no single test that confirms bird fancier's lung on its own. Diagnosis is built from several pieces of evidence used together. The starting point is always a thorough exposure history, often guided by a validated questionnaire that asks about birds, feather-containing items, mold, and other known HP triggers.
Serum IgG testing (sometimes called precipitin testing) looks for antibodies against specific avian antigens in your blood. A positive result supports the diagnosis but does not confirm it on its own, since some exposed people develop antibodies without getting sick. A negative result does not fully rule it out either.
Imaging plays a major role. A high-resolution CT scan (HRCT) of the chest can show characteristic patterns linked to HP, including ill-defined centrilobular nodules, ground-glass opacity, air trapping, and a specific 'three-density pattern' of mosaic attenuation. These patterns help distinguish HP from other interstitial lung diseases and from infection.
Bronchoalveolar lavage (BAL), where fluid is washed into the airway and analyzed, often shows a high proportion of lymphocytes in HP, which supports the diagnosis and helps exclude infection or malignancy. In unclear or more advanced cases, a surgical lung biopsy may be needed to reach a definitive answer and determine whether fibrosis is present.
It is worth knowing that bird fancier's lung shares symptoms with other bird-related respiratory illnesses. Psittacosis, for example, is a bacterial infection from birds (particularly parrots and pigeons) that also causes fever, cough, and lung inflammation but requires antibiotic treatment rather than antigen avoidance. Getting the right diagnosis matters because the treatment paths are different.
Treatment options and what to realistically expect

Antigen avoidance is the cornerstone of treatment, not a secondary step. The American Lung Association and clinical guidelines all agree: identifying the source and eliminating exposure is the most important intervention. For many people with nonfibrotic disease, doing this early is enough for the lungs to recover.
When symptoms are severe, lung function is significantly impaired, or imaging shows extensive involvement, doctors typically prescribe systemic corticosteroids such as prednisone. A common approach is prednisone at around 0.5 mg/kg per day for one to two weeks, followed by a gradual taper over several weeks to a maintenance dose of around 10 mg/day. Steroids speed up the initial recovery but they do not replace the need to eliminate exposure. Inhaled steroids are not an effective substitute for systemic ones in this condition.
For patients who relapse, progress despite steroids, or cannot tolerate long-term corticosteroids, steroid-sparing medications like azathioprine or mycophenolate mofetil may be added. In chronic cases where fibrosis is progressing despite antigen removal and anti-inflammatory treatment, antifibrotic agents have been considered as part of management.
| Disease Stage | Fibrosis Present? | Recovery Potential | Main Treatment Focus |
|---|
| Acute (nonfibrotic) | No | Full recovery likely with prompt exposure removal | Stop exposure; steroids if severe |
| Subacute (nonfibrotic) | No | Good recovery if exposure stopped; some residual symptoms possible | Stop exposure; steroids if needed; monitor lung function |
| Chronic (nonfibrotic) | No | Partial to good recovery possible; depends on antigen burden removed | Sustained exposure elimination; anti-inflammatory treatment |
| Chronic (fibrotic) | Yes | Irreversible; goal is to stop further decline | Remove ongoing exposure; anti-inflammatory or antifibrotic agents; close monitoring |
One study found that the amount of avian antigen remaining in household dust directly predicted prognosis in chronic bird-related HP. This means that incomplete antigen removal, where you reduce but do not eliminate exposure, can continue driving disease even while you are being treated.
Steps to take right now to stop exposure
This is the part that requires the most practical action. Stopping exposure means more than just moving the bird to another room. Avian antigens are microscopic proteins that circulate through air, settle into dust, and embed in soft furnishings. Even after birds are removed from a home, antigen levels can remain elevated for weeks if the environment is not cleaned properly.
- Separate yourself from all birds immediately, either by rehoming them, moving them to a separate building, or having someone else care for them while you seek medical evaluation.
- Remove all feather-containing items from your sleeping area and ideally from the home entirely: down pillows, feather duvets, feather-stuffed couch cushions, and similar products.
- Clean the environment thoroughly using HEPA-filtered vacuums and wet-wiping surfaces. Standard vacuuming can stir antigens back into the air.
- Improve ventilation in rooms where birds have been kept. Open windows and use air purifiers with HEPA filters.
- Wash all soft furnishings, curtains, and bedding that may have accumulated bird dust.
- Have someone else handle bird care tasks like cage cleaning if the birds cannot be rehomed immediately, since cage cleaning generates the highest antigen concentrations.
- Avoid feather-containing items even when visiting other homes or staying in hotels, as some people react to down pillows and duvets even without pet bird contact.
If rehoming birds feels like a difficult decision, it is worth knowing that repeated antigen exposure is associated with irreversible fibrosis. The longer avian protein exposure continues after diagnosis, the greater the risk of permanent lung damage. That context often makes the decision clearer.
Preventing recurrence if you stay involved with birds
For people who work with birds professionally or continue bird-related activities after recovery, preventing recurrence requires sustained and deliberate exposure management. The immune system in someone with bird fancier's lung will react again to the same antigens, sometimes more severely than the first time.
- Use a properly fitted respirator (N95 or better) when handling birds, cleaning cages, or being in dusty bird environments. A standard dust mask is not adequate.
- Keep birds out of living areas and sleeping spaces entirely, even if you feel fully recovered.
- Use HEPA air purifiers continuously in any rooms shared with birds.
- Have the antigen levels in your home environment checked or reassessed if symptoms return.
- Schedule regular follow-up appointments with a pulmonologist to monitor lung function, especially if your work involves ongoing bird contact.
- Know your early warning symptoms and act on them immediately rather than waiting to see if they resolve on their own.
- Inform household members about the risks, since other people living in the home can also develop bird fancier's lung from the same environment, and their exposure should be assessed too.
It is also worth ruling out whether other bird-related conditions are contributing to your symptoms. The symptoms of bird fancier's lung overlap with conditions like psittacosis (a bacterial bird illness that can infect people) and other forms of hypersensitivity pneumonitis from non-avian sources. Getting a precise diagnosis from a pulmonologist or interstitial lung disease specialist ensures you are treating the right problem.
The bottom line: bird fancier's lung can be cured in the sense that full lung recovery is genuinely possible when exposure is stopped early and fibrosis has not developed. Because it can be irreversible once fibrosis develops, bird fancier's lung may be fatal if exposure continues and the disease progresses. But it requires action, not watchful waiting. The earlier you remove the antigen, get properly diagnosed, and follow through with treatment, the better your chances of getting your lung function back to normal.