If you're searching 'bird nest vs cancer,' you're probably trying to figure out whether a lump, swelling, or abnormal growth you've noticed on your bird is something serious or something that can wait. The honest answer is: you can't tell for certain at home, but you can gather enough information right now to know whether this is a same-week vet visit or a get-to-an-avian-vet-today situation. Most lumps in birds are not cancer, but some are, and the ones that are caught early have better outcomes. Here's exactly what to look for and what to do next.
Bird Nest vs Cancer: Symptoms and What to Do Now

What 'bird nest vs cancer' probably means
This search phrase is almost always shorthand for a real concern: a bird owner has spotted something unusual, maybe near where a bird nests or breeds, maybe on the bird's body itself, and they're trying to figure out if it's cancer or something more benign. Sometimes it comes up in the context of a nest-bound or brooding bird showing physical changes that worry an owner. Occasionally, 'bird nest' refers to edible bird's nest used in traditional wellness contexts, but on a health site focused on avian illness, the most practical interpretation is a worried bird owner looking at an abnormal mass, swelling, growth, or tissue change and trying to make sense of it.
Avian cancer is real and more common than many people realize. According to Merck's veterinary resources, neoplasia (abnormal tissue growth) occurs with some frequency across pet birds of all ages, and incidence is likely to rise as birds live longer. Tumors can appear on the skin, in the sinuses, oral cavity, GI tract, lungs, air sacs, liver, spleen, kidneys, and the reproductive tract. Lymphoma is the most common lymphoid cancer seen in psittacine and passerine birds. So while cancer is genuinely on the differential list, it's far from the only possibility, and that's worth keeping in mind before you spiral.
Cancer-like growths vs benign causes: what actually looks similar

A visible lump or swelling on a bird can come from a surprisingly long list of causes, and the appearance alone rarely tells you which one you're dealing with. That's what diagnostics are for. But knowing the range helps you have a more productive conversation with your vet and stops you from assuming the worst immediately.
Signs that raise concern for cancer
- A firm, fixed, or rapidly growing lump that doesn't move easily under the skin
- Skin discoloration, ulceration, or a mass around the eyes, beak, wing tips, or toes (squamous cell carcinoma is known to appear in these locations)
- Unexplained weight loss, especially loss of pectoral muscle mass (the breast feels sharp or 'keel-like' instead of rounded)
- Persistent lethargy, fluffed feathers, and a bird that's stopped being its normal self over days or weeks
- Swelling in the abdomen that doesn't resolve and isn't explained by egg-binding or normal breeding activity
- Breathing changes: wheezing, tail bobbing while at rest, or open-mouth breathing, which can indicate a mass is affecting the airway or air sacs
- Feather changes or abnormal plumage growth around a localized area without a clear skin infection cause
Benign causes that look just as alarming
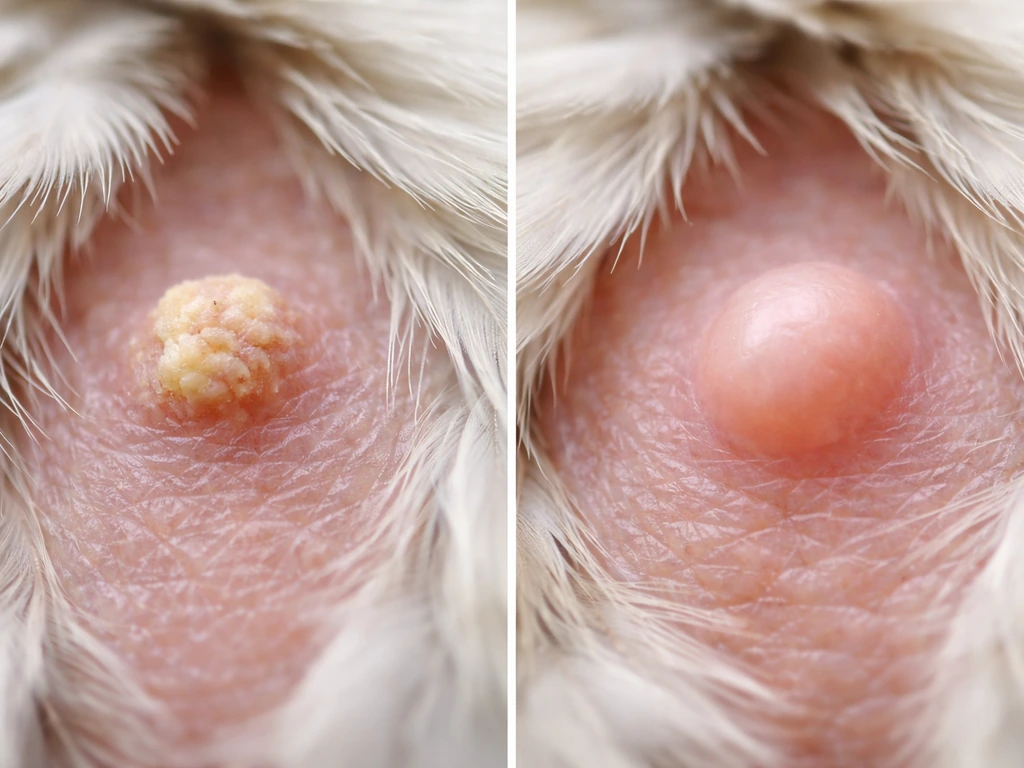
- Abscesses or infections: birds don't produce liquid pus the way mammals do; avian abscesses are often firm and caseous (solid), making them look and feel a lot like tumors
- Cysts: feather cysts, especially in canaries and some softbills, can grow large and look frighteningly like masses
- Lipomas: soft, movable fatty deposits are very common in overweight birds, especially budgerigars and Amazon parrots, and are usually benign
- Trauma or wound-related swelling: a bite, cage injury, or impact can cause localized swelling that mimics a growth
- Parasitic granulomas: certain parasites can trigger inflammatory masses under the skin
- Egg-related issues: egg binding, retained eggs, or reproductive tract problems in female birds can cause abdominal swelling that has nothing to do with cancer
- Respiratory infections or sinusitis: swelling around the sinuses or face from bacterial or fungal infections can look like a tumor from the outside
The overlap between these categories is exactly why you can't rely on appearance alone. A firm facial swelling could be a sinus abscess from a bacterial infection or a squamous cell carcinoma. You genuinely need a vet to tell you which.
A safe at-home check you can do right now
Before you handle your bird extensively, do a visual assessment first. Birds under stress from handling can deteriorate quickly, especially if they're already unwell, so observe from a short distance and limit physical contact until you know what you're dealing with.
What to observe without picking the bird up
- Breathing: Is the bird breathing with its mouth open at rest? Is its tail bobbing rhythmically up and down with each breath? Is the chest or body moving more than usual? Any of these, especially open-mouth breathing or tail bobbing, are red flags that need same-day veterinary attention. These signs suggest either the airway is compromised or the bird is in respiratory distress.
- Posture and perching: Is the bird sitting on the cage floor instead of a perch? Is it hunched with feathers fluffed? A bird that can't or won't perch is telling you something is seriously wrong.
- Alertness: Does the bird respond normally to sound and movement? A bird that's dull, unresponsive, or closing its eyes when it normally wouldn't is showing signs of systemic illness.
- Appetite and droppings: Has it been eating and drinking? Are droppings normal in color, consistency, and frequency? Changes in droppings, including very watery or discolored ones, can indicate internal disease.
- Visible mass or swelling: Note the location (head, neck, abdomen, wing, leg, vent area), size (roughly how large), texture if observable (smooth, lumpy, ulcerated), and whether the overlying skin or feathers look abnormal.
If you do handle the bird briefly
If your bird is tame enough to hold safely and you need to assess the mass, keep it brief. Gently feel whether the lump is soft or firm, movable or fixed, and whether touching it causes the bird obvious distress. Check the breast muscle: a healthy bird should have well-rounded pectoral muscles on either side of the keel bone. If the keel feels prominent and sharp, the bird has likely lost significant body condition, which is a meaningful clinical sign regardless of what's causing it.
When to stop the home assessment and call a vet immediately
Go straight to an avian vet or emergency clinic if you see open-mouth breathing at rest, pronounced tail bobbing, wheezing, blue or pale tissues around the beak or face, collapse, inability to stand or perch, seizures, or uncontrolled bleeding. These are not watch-and-wait situations. Respiratory distress in particular can deteriorate very fast in birds.
What a vet will actually do to tell cancer from something else
An avian vet's diagnostic process is systematic and doesn't jump straight to assuming cancer. Here's roughly how it unfolds.
Physical exam and palpation
The vet will assess the bird's overall condition, including body weight, muscle mass, hydration, and mucous membrane color. They'll palpate the mass carefully, noting size, texture, mobility, temperature, and whether the bird reacts to pressure. They'll also evaluate the respiratory rate and any signs of distress, and assess the abdominal cavity, crop, and vent area depending on where the concern is.
Cytology via fine needle aspiration (FNA)
For accessible surface masses, fine needle aspiration is often the first sampling step. A thin needle is inserted into the mass to collect cells, which are then stained and examined under a microscope. This can quickly distinguish between infection, inflammation, lipoma, cyst, and malignant cells in many cases. It's minimally invasive and gives the vet a lot of useful information fast. Avian clinicians also use squash preparations and cloacal or fecal cytology as part of a broader evaluation.
Biopsy and histopathology

When cytology is inconclusive or when a definitive diagnosis is needed before committing to treatment, a biopsy is the next step. A small tissue sample is submitted to a pathology laboratory for full histopathological analysis. This gives the most reliable cancer versus non-cancer answer and, if cancer is confirmed, helps determine the tumor type and grade.
Imaging and bloodwork
Radiographs (X-rays) and, where available, CT scans or ultrasound help assess internal masses, organ involvement, and whether a growth has spread. Bloodwork, including a complete blood count and biochemistry panel, evaluates organ function and looks for systemic signs of disease. Endoscopy can be used for internal visualization and to collect tracheal or other internal samples for cytology and culture, which is especially useful when differentiating neoplasia from respiratory infection or inflammation.
When urgency really matters
If the mass is affecting breathing, causing visible distress, growing very rapidly, or is located near critical structures like the airway or major blood vessels, the diagnostic timeline compresses significantly. Don't wait for a routine appointment if any of those apply. Same-day or next-day evaluation is appropriate.
Treatment options and realistic outcomes
If diagnostics confirm cancer, the treatment path depends heavily on the tumor type, location, extent, and the bird's overall health. Avian oncology is a genuinely developing field, and outcomes vary considerably. Here's what's currently available.
| Treatment Option | When It's Used | Realistic Expectation |
|---|---|---|
| Surgical removal | Accessible, localized tumors (skin, reproductive tract, some internal masses) | Can be curative if margins are clean and the tumor hasn't spread; recovery depends on the bird's condition and tumor location |
| Chemotherapy | Lymphoma and some other systemic cancers in birds | Has been used successfully in birds; protocols are adapted from mammalian medicine and response varies by individual and tumor type |
| Radiation therapy | Selected cases, often in combination with other treatment | Used in some avian oncology centers; can be effective for lymphoma; access is limited by availability of specialized equipment |
| Medical management | Hormone-responsive tumors, some reproductive cancers | Leuprolide acetate and similar agents can manage reproductive tumors in some birds without surgery |
| Palliative and supportive care | Advanced disease, poor surgical candidates, owner choice | Focuses on comfort, pain management, and quality of life; can extend good-quality time even when cure isn't possible |
| Euthanasia (comfort-first decision) | Severe suffering, no viable treatment, rapidly declining quality of life | A legitimate and compassionate option; avian vets will discuss this honestly when it becomes relevant |
Prognosis is genuinely hard to generalize. A small, surface lipoma removed cleanly has an excellent outcome. A diffuse internal lymphoma detected late carries a much more guarded one. The most honest thing a vet can tell you depends on what the diagnostics show, so the faster you get answers, the more options you typically have.
Benign findings and supportive care while you wait for answers
Many birds that present with a suspicious mass turn out to have something treatable and non-cancerous. Abscesses respond to surgical debridement and antibiotics. If an infection in your bird suggests bacterial involvement, ask your vet whether any sulfa therapy is appropriate and how dosing should be calculated for your pet bird sulfa dosage for dogs. Feather cysts can be surgically removed. Lipomas in overweight birds often respond to dietary changes, and some regress significantly with improved nutrition alone. Reproductive swellings from egg binding or related issues are addressed with specific interventions for those conditions.
While you're waiting for a vet appointment, focus on keeping your bird comfortable and stable. Maintain a warm, stress-free environment (around 85 to 90 degrees Fahrenheit if the bird appears ill and cold). Jade bird side effects are not something to guess at, because individual supplements and dosing can affect birds differently. Make food and water easily accessible, especially if the bird seems weak. Avoid unnecessary handling. Don't try to drain or manipulate the mass yourself. Keep other pets away. If you notice breathing changes, escalate immediately rather than waiting. If you want to explore supportive options for cough, talk with an avian vet first, because the use of bird nest products depends on the bird and the cause of the cough bird nest good for cough.
It's also worth knowing that supportive nutrition and husbandry play a real role in how birds tolerate illness and recovery. Ensuring your bird is on a balanced diet before any illness crisis is one of the most impactful things you can do for long-term health. Is bird nest good for eczema? The evidence is limited, so treat it as an unproven remedy rather than a substitute for vet guidance and proven eczema care. If your bird has respiratory concerns alongside a suspicious mass, it's useful to know that the relationship between avian respiratory health and overall systemic illness is closely connected, something covered in more detail in discussions of bird nest benefits for lungs and bird nest good for cough topics. If you're considering HUM skinny bird side effects or edible bird's nest wellness products, it's smart to check how respiratory and systemic health could be affected bird nest benefits for lungs.
Reducing the risk: practical prevention and early detection habits
You can't eliminate every cancer risk in a bird, but you can significantly reduce exposure to known contributing factors and catch problems earlier when outcomes are better.
Environment and toxin reduction
- Keep birds away from non-stick cookware fumes (PTFE/Teflon), cigarette smoke, air fresheners, scented candles, and aerosol sprays, all of which can damage avian respiratory and cellular health
- Ensure the aviary or cage is well-ventilated but free from drafts, and cleaned regularly to reduce bacterial and fungal load
- Avoid zinc and lead exposure from old paint, galvanized wire, or certain toys and hardware, as heavy metal toxicity can have overlapping symptoms with tumor-related illness
- Use bird-safe cleaning products and rinse all surfaces thoroughly before returning your bird to the enclosure
Nutrition and weight management
- A pellet-based diet supplemented with fresh vegetables and appropriate fruits reduces the risk of obesity-related lipomas and supports immune function
- Avoid high-fat seed-only diets, which are strongly associated with lipoma development in budgerigars and Amazon parrots
- Maintain a healthy body weight: obese birds have higher rates of fatty tumors and reproductive cancers
Managing breeding and nesting safely
For female birds, chronic egg laying significantly increases the risk of reproductive tract problems including tumors. If your bird is a persistent egg layer, talk to an avian vet about hormonal management options before a problem develops. Avoid over-stimulating breeding behaviors with excessive nest boxes, long light cycles, or nesting materials if you're not actively breeding.
Routine monitoring and check-ups
Annual wellness exams with an avian-experienced vet are one of the most effective early detection tools available. Birds hide illness instinctively, so by the time symptoms are obvious, disease can be well advanced. A vet can detect subtle changes in body condition, palpate for early masses, and run baseline bloodwork that makes future comparisons meaningful. In between visits, do a brief weekly visual check at home: watch your bird eat, observe its posture and breathing, and note any new lumps, feather changes, or behavioral shifts. Document what you see. Catching a 1-centimeter mass before it becomes 3 centimeters genuinely changes the conversation about what's possible.
FAQ
How quickly should I go to the vet if the “lump” might be cancer?
If the mass is growing fast, changing over days, affecting breathing, or you see weakness like inability to perch, you should use same-day or next-day evaluation. For a stable lump that is not causing distress, book an avian vet visit soon rather than waiting weeks, because cytology or imaging work is time-sensitive once a lesion affects organs.
What’s the difference between a skin mass and an internal tumor, and does it change what the vet does first?
Skin and visible surface lesions are often sampled early with fine needle aspiration, while suspected internal masses may require radiographs first and then CT, ultrasound, or endoscopy depending on location. If you cannot clearly see a boundary between the mass and normal tissue, assume it might be deeper and avoid delay.
Can I take a photo or video at home to help the vet diagnose sooner?
Yes, photos and short videos can speed triage. Take images from the same angles with good lighting, record the size relative to a known object (like the bird’s band size or a ruler placed outside the cage), and note breathing rate, tail bobbing, and whether the bird reacts when you approach.
Is fine needle aspiration safe for birds, and should I ask my vet about it?
In many cases it is minimally invasive and helps distinguish infection, cyst, inflammation, and malignant cells quickly. Ask your avian vet what sampling method is safest for your bird’s size and mass location, especially if the lesion is near the airway or major vessels.
If the cytology is negative, does that rule out cancer?
Not always. Sampling can miss cancer if the lesion is heterogeneous or the needle targets a non-representative area. If the lesion keeps enlarging, becomes fixed, or your bird’s condition worsens, ask about repeat sampling, biopsy, or imaging even after an inconclusive result.
My bird is still eating, does that mean the mass is probably not cancer?
Not necessarily. Many birds compensate until disease is advanced, and cancer and chronic infections can start with subtle changes. Body condition and breathing are more informative than appetite alone, so still pursue evaluation if the mass persists or grows.
What signs tell me the mass is more urgent than “wait and see”?
Treat it as urgent if there is open-mouth breathing at rest, wheezing, bluish or very pale tissues around the beak, collapse, seizures, uncontrolled bleeding, inability to perch, or rapid growth. Also escalate if the bird is guarding the area strongly or shows marked pain with minimal contact.
Should I warm my bird to 85 to 90 F if they have a suspected mass?
Only if the bird seems cold or ill and is not actively overheating. Birds with respiratory distress can fatigue quickly in a stressful environment, so focus on gentle warmth, quiet, and easy access to food and water, and confirm guidance with an avian vet if you are unsure.
Can I use supplements or edible bird nest products while waiting for the appointment?
Avoid starting new supplements or wellness products without vet input, because some additives can interact with illness, appetite, or supportive medications. If you are considering any “bird nest” product specifically for cough or respiratory support, ask the avian vet first and do not treat it as a substitute for diagnosis.
Is it okay to drain or massage the lump at home if it seems like a cyst?
No. Manipulating or attempting to drain can cause bleeding, spread infection, or damage underlying tissue and make later biopsy or surgery harder. Do only brief, careful visual and light palpation to assess firmness and mobility, then let the vet decide on sampling.
How can I estimate whether the bird is losing condition, and why does it matter?
Check the keel bone prominence and the overall contour of the breast muscles. A sharp or very prominent keel plus reduced muscle “fill” suggests weight loss or chronic disease, which can affect both treatment options and urgency regardless of whether the cause is cancer, infection, or another disorder.
What husbandry details should I tell the vet to help narrow causes?
Share whether the bird is a persistent egg layer, any recent changes in diet or supplements, nesting or breeding conditions (nest boxes, long light cycles), and whether the mass is near the face, sinuses, crop, vent, or limbs. These details can shift the differential diagnosis toward reproductive, infectious, or tumor-related causes.
If cancer is confirmed, what questions should I ask right away?
Ask for the tumor type and grade if available, whether it appears localized or has spread, expected treatment options (surgery, chemotherapy, radiation if offered, or palliative care), and likely timelines for response. Also ask what monitoring signs to watch at home and how soon you should recheck after starting treatment.
How often should I do at-home monitoring once a lump is found but before the appointment?
Do a brief weekly visual check at minimum, but if you notice any growth or behavior change, reassess daily and document it. Track breathing quality and posture, and write down whether the lump’s size, firmness, or location relative to feathers changes over time.
Citations
Merck notes that avian cancer/tumors can involve many locations, including skin (notably squamous cell carcinomas around eyes/beak, wing tips, toes), sinuses, oral cavity, GI tract, lungs/air sacs, liver/spleen/kidneys, and the reproductive tract.
https://www.merckvetmanual.com/bird-owners/disorders-and-diseases-of-birds/cancers-and-tumors-of-pet-birds
Merck describes that neoplasia occurs with some frequency in pet birds of all ages and includes cancer of multiple organ systems; it also states incidence of cancer is likely to rise as pet birds age.
https://www.merckvetmanual.com/exotic-and-laboratory-animals/pet-birds/neoplastic-diseases-of-pet-birds
A presenting-problem/clinical education article on Lafeber emphasizes that diffuse disease or large focal lesions can obstruct the upper airway/choanal slit and/or glottis, leading to wheezing or open-mouth breathing in severe cases (relevant to mass vs cancer vs infection confusion when breathing changes occur).
https://www.lafeber.com/vet/content_types/presenting-problem/
Merck’s general avian illness guidance specifically lists breathing difficulties (e.g., wheezing or tail bobbing while breathing) as signs to monitor—important for “tumor vs benign swelling” scenarios that affect respiration.
https://www.merckvetmanual.com/bird-owners/routine-care-and-safety-of-birds/illness-in-pet-birds
PennVet’s avian triage material identifies tail bobbing and open beak/breathing as critical respiratory signs in avian patients (useful as a “mass is affecting breathing” red-flag pathway).
https://www.vet.upenn.edu/docs/default-source/penn-annual-conference/pac-2019-proceedings/companion-animal-track-2019/nursing-track-tue-2020/liz-vetrano---the-avian-triage.pdf?sfvrsn=9af6f2ba_2
LafeberVet states observable dyspnea signs in birds include open-mouth breathing, increased sternal motion, and tail bobbing.
https://lafeber.com/vet/respiratory-emergencies/
Merck says lymphoma/lymphosarcoma is the most common lymphoid neoplasia in psittacine and passerine birds, and that primary respiratory neoplasia is uncommon in psittacines except for a mixed pulmonary tumor reported in cockatiels.
https://www.merckvetmanual.com/exotic-and-laboratory-animals/pet-birds/neoplastic-diseases-of-pet-birds
Merck notes that surgery and chemotherapy have been used with varying success depending on tumor location and extent; it specifically mentions radiation and chemotherapy used successfully for lymphoma in birds (general therapeutic pathway reference).
https://www.merckvetmanual.com/bird-owners/disorders-and-diseases-of-birds/cancers-and-tumors-of-pet-birds
IVIS describes that internal samples (e.g., tracheal exudates when present) can be collected for cytology and culture during endoscopy/diagnostics, helping differentiate neoplasia vs infection/inflammation.
https://www.ivis.org/library/clinical-avian-medicine/diagnostic-value-of-endoscopy-and-biopsy
VCA explains that cytology is commonly obtained via fine needle aspiration (FNA) from a growth/tumor; aspirated cells are then stained and examined under a microscope to classify cells as normal vs abnormal.
https://www.vcahospitals.com/premier/know-your-pet/testing-and-diagnostics-for-sick-pet-birds
VCA distinguishes that a biopsy is tissue sampling submitted to a laboratory for pathologist evaluation; it also notes cytology can be used for on-the-spot assessment during surgery when a mass is found.
https://www.vcahospitals.com/know-your-pet/cytology-histopathology-biopsies
dvm360 provides that avian clinicians often rely on hematologic/biochemical/cytologic/immunologic tests; it also notes common sampling methods for internal organs include aspiration/squash preparations and that cloacal/fecal cytology is used as a routine part of the physical exam.
https://www.dvm360.com/view/guidelines-important-evaluating-cytological-samples-birds
Merck’s routine care illness page lists key assessment behaviors (including monitoring breathing and mentation/posture) that caretakers can apply immediately while preparing for veterinary evaluation.
https://www.merckvetmanual.com/bird-owners/routine-care-and-safety-of-birds/illness-in-pet-birds
Merck includes monitoring guidance such as observing respiratory rate/effort and the presence of open-mouth breathing, along with mentation/alertness and posture (e.g., tail bobbing, wing position) before/without extensive handling.
https://www.merckvetmanual.com/exotic-and-laboratory-animals/pet-birds/management-of-pet-birds
A technician/clinical program handout lists that avian emergency assessment includes a rapid physical exam and systematic evaluation including assessment of pectoral muscle mass to guide body condition.
https://www.mmhimages.com/production/Creative/1OldBackup/fetch_Backup/CVC_DC_2014_proceedings_proof/data/PDFs/Technician%20Program/Heard/Heard_Darryl_Management.pdf
SpectrumCare lists emergency care as warranted for open-mouth breathing, pronounced tail bobbing, wheezing, blue or very pale tissues, collapse, seizures, uncontrolled bleeding, severe trauma/burns/toxin exposure, or sudden inability to stand/perch.
https://spectrumcare.pet/birds/care/bird-emergency-vet
LafeberVet’s client-education PDF flags open-mouthed breathing at rest as very serious, and tail bobbing as a key observable sign needing immediate veterinary attention.
https://lafeber.com/vet/wp-content/uploads/Signs_of_Illness.pdf
The PDF includes a “no breathing or difficulty breathing” warning listing open-mouth breathing and tail bobbing while breathing as reasons to seek veterinary help.
https://cdn.ymaws.com/petsitters.org/resource/resmgr/virtual_library_/signs_of_diseases_in_birds.pdf
PetPlace notes dyspneic birds often breathe with mouths open and may show whole-body breathing effort including tail bobbing; it states any bird appearing to have difficulty breathing should be seen by a veterinarian.
https://www.petplace.com/article/birds/general/dyspnea-in-birds
Not provided—ignore.
https://www.wsonline.com/
Bird Nest for Cough: Does It Help and When to See a Vet
Find out if bird nest helps a cough in birds, safe use tips, and urgent vet signs when home care won’t work.


